THEY were four deaths of children and teenagers between 1999 and 2007 that shocked the community and exposed significant failings in how Central Coast public hospitals responded to meningococcal cases.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Charissa Tsouvallas, 18, Stephen Sanig, 7, Rebecca Calverley, 7, and Gabrielle Coventry, 14, died at Gosford and Wyong hospitals in that eight year-period from a disease that remains notoriously difficult to diagnose and still has a fatality rate of 5-10 per cent despite advanced treatment.
Coroners later found their deaths were “preventable”, hospital staff and doctor failures were “inexcusable” and “catastrophic”, clear warning signs were missed or ignored and parents’ desperate pleas for help and treatment in their children’s final hours were dismissed by staff. In Stephen Sanig’s case a dying child was sent home with painkillers.
Now questions are being asked by Stephen’s father, Michael Sanig, and Wyong MP David Harris after the death of Mischelle Rhodes, 19, at Gosford Hospital on August 29. The Macquarie University student died of the meningococcal W strain a day after she was seen by Gosford Hospital emergency department staff and sent home with painkillers. She was later admitted after her symptoms worsened but died despite aggressive treatment.
Central Coast Local Health District said it is reviewing details of the case as part of its standard processes.

But Mr Harris and Mr Sanig say an independent external review is needed because of public concern about the health system’s ability to respond to meningococcal disease; data showing the mortality rate for children and teenagers with meningococcal disease is higher in disadvantaged areas and the health region’s meningococcal history.
Mr Harris supported Michael Sanig and his former wife Sue-Anne’s long campaign to improve public understanding of meningococcal and the health system’s response to it after Stephen’s death in June, 2001. He acknowledged the majority of meningococcal cases were appropriately diagnosed and treated, with good outcomes.
But the reported circumstances of Ms Rhodes’ death at a hospital with Gosford’s history meant the community was entitled to an independent rather than a hospital-led review to provide confidence in the public health system, he said.
The deaths of Charissa Tsouvallas in 1999, Stephen Sanig in 2001, Rebecca Calverley in 2002 and Gabrielle Coventry in 2007, and subsequent inquests exposing significant failings, meant Central Coast hospitals should be best placed to respond to meningococcal because of lessons learnt, Mr Harris said.

“Once or twice (to have problems leading to meningococcal deaths) then maybe it’s the nature of the condition itself, but those four cases show we think it does need to be looked at more carefully after this latest tragic case.”
Mr Sanig said he was “a bit shocked” to learn of Ms Rhodes’ death under circumstances similar to his son’s death 17 years ago.
“The young woman has apparently presented with certain symptoms and was sent home. If somebody presents with symptoms severe enough that they go to a hospital emergency department then you should say there’s a possibility it might be meningococcal so let’s err on the side of caution,” Mr Sanig said.
“You would have thought by now everybody would err on the side of caution. Why wasn’t she given antibiotics as a precautionary measure?”
Ms Rhodes is the second Central Coast person to die of meningococcal this year after a woman, 38, died of the meningococcal W strain during an overseas trip. A third Central Coast person has also recovered from the disease in 2018.
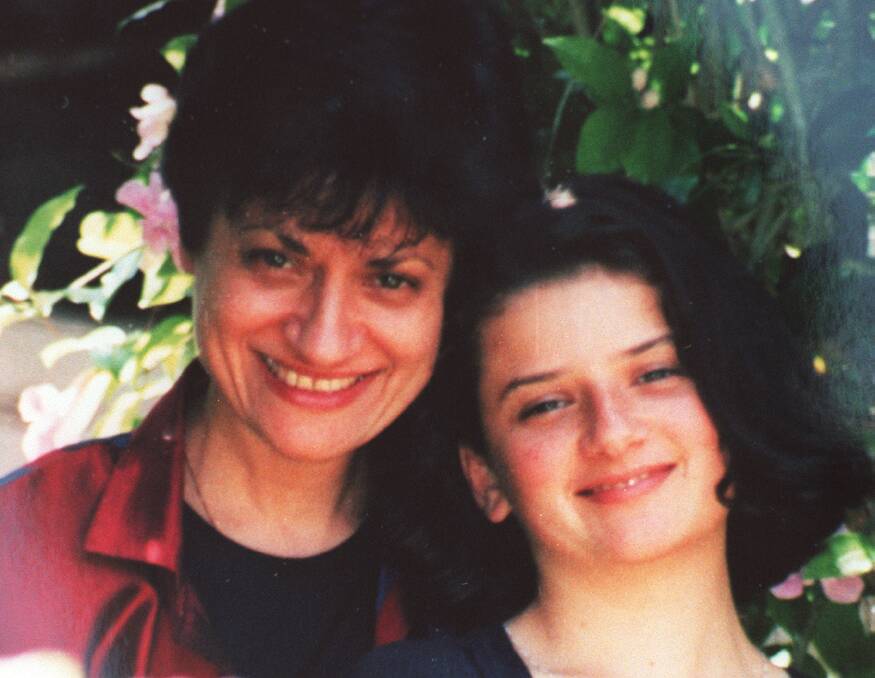
A NSW Health spokesperson said there have been 41 meningococcal cases across NSW in 2018, and 91 cases in 2017, with meningococcal B the most dominant strain.
Despite public concern about the relatively high meningococcal mortality rate it remains very uncommon in NSW because the bacteria is not easily spread from person to person, Central Coast Local Health District director of public health Dr Peter Lewis said.
A National Centre for Immunisation Research and Surveillance report to NSW Parliament in 2016 found there were 26 deaths in NSW children aged 15 or younger between 2000 and 2007, during a period that largely predated most meningococcal vaccinations. There were 12 meningococcal child deaths between 2005 and 2014 after meningococcal C vaccinations were available from 2003 but before meningococcal B vaccinations in 2014, and combined ACWY strain vaccinations.
Inquests into the deaths of the four Central Coast children and teenagers found disturbing communication breakdowns and difficulties between hospital staff, between staff and parents and between hospitals and general practitioners. It also found warnings were missed because staff were busy.
Julie Calverley urged parents to “Don’t worry about looking stupid. Just get up and shout, ‘This is my kid. Fix it’,” after she waited for six hours with daughter Rebecca in a busy Wyong Hospital emergency department in July, 2002 until rashes on the child’s body showed meningococcal.

Mrs Calverley said she sat quietly for hours after arriving at the hospital at 8.30pm because she assumed if doctors were slow to attend to her daughter it must have meant her illness was not serious.
Charissa Tsouvallas, 18, died at Gosford Hospital in July, 1999 more than a week after blood tests ordered by the hospital showed an excessively high white blood cell count that “should have rung alarm bells” but of a serious bacterial infection, her inquest was told. A Gosford Hospital doctor did not give the tests “even a cursory glance” when Charissa returned to the hospital with worsening symptoms. She died only days after her 18th birthday.
Her mother Terry was devastated when a coroner concluded her daughter’s death was “preventable”.
“It is really hard for me to go past those words,” Mrs Tsouvallas said.
Michael and Sue-Anne Sanig were shattered after a coroner found doctors who clearly made mistakes in the treatment of their son Stephen in June, 2001 refused to accept they were wrong despite being challenged at his inquest.
“While hindsight is a wonderful thing, clearly in the case of Stephen Sanig mistakes were made at Gosford Hospital which should not have been made,” coroner Michael Morahan said.
Gabrielle “Gabi” Coventry died in Gosford Hospital in December, 2007 despite her mother’s desperate appeals for help and was “doomed” because of a “cascading series of systematic and individual errors”, a coroner found after her inquest in 2011.

She died after “inexcusable” failures at the hospital, including doctors who became “fixated” on a diagnosis linked to a single sexual incident, and despite eight doctors being involved in her care in the final 15 hours of her life. Her hospital notes showed her mother was distressed and appealed for antibiotics for her only daughter.
Central Coast Local Health District chief executive Dr Andrew Montague said Ms Rhodes’ death was an “absolute tragedy” and the hospital was communicating with her family as it reviews management of her treatment.
The Central Coast has had 33 reported cases of meningococcal disease between 2009 and 2018 and four deaths during that period, including a woman who died of the condition while travelling overseas this year.
The number of cases and deaths was statistically average, Dr Montague and Dr Lewis said.
The Central Coast health service and NSW Health in general had not only learnt from the tragic Central Coast deaths between 1999 and 2007 but had made significant changes to protocols and procedures for managing patients, including formal clinical handovers to ensure clear lines of responsibility for patients, they said.
Central Coast Health has also doubled emergency department staff and provides round-the-clock pathology services at Wyong Hospital, after staff resourcing was raised at the earlier inquests.
The Central Coast’s meningococcal immunisation rates for babies, children and teenagers is also high, with more than 95 per cent of babies immunised and more than 70 per cent of teenagers in school programs for years 10, 11 and 12. Immunisation was one of the major reasons meningococcal numbers are falling across the state, Dr Lewis said.
Dr Montague said the hospital agreed that transparency was necessary to ensure public confidence in the health system.
“We don’t shy away when bad things have happened because it’s important the community knows,” Dr Montague said.
Symptoms of meningococcal disease include sudden onset of fever, headache, neck stiffness, joint pain, a dislike of bright lights, nausea and vomiting, with a rash of red-purple spots or bruises generally after the disease has progressed to a serious degree, although 25 per cent of people do not experience a rash.

